Dealing with Pressure: Surgical Coping Strategies for Cataract Surgeons
The Stage Fright of the Scalpel: What Surgeons Can Learn from Elite Athletes and Rock Stars
The water runs hot, the chlorhexidine lathers, and for three minutes, the world narrows to the rhythmic friction of bristles against skin. In the surgical theater, “scrubbing up” is ostensibly about antisepsis, but for the seasoned clinician, it is a psychological airlock. It is the threshold between the mundane world and a high-pressure stage where the stakes are measured in human life. Even for the most elite, this threshold can be haunted by a silent companion: performance anxiety.
Performance anxiety (PA) is often misunderstood as a tremor of the novice, yet it is an evolutionarily adaptive reflex—a “perceived threat concerning the performance of a task under pressure”—that facilitates protective autonomic responses. In the operating room, where perfection is not an aspiration but the baseline, this anxiety can shift from a motivational spark to a maladaptive weight. To understand how to manage it, we must look beyond the medical literature to the concert halls and athletic stadiums, where the psychology of elite performance has long been deconstructed.
The “Audience” in the Operating Room
We often imagine the surgeon as a solitary figure of stoic concentration, but the reality is far more communal. A surgeon performs in a fishbowl, observed by an “audience” of registrars, anaesthetists, and scrub nurses. This social-evaluative threat—the fear of being judged by one’s peers—is perhaps the most potent catalyst for PA.
The scale of this burden is best illustrated by our counterparts in the arts. In a landmark survey of 56 world-class orchestras, a staggering 70% of musicians reported experiencing performance anxiety severe enough to impair their artistry. Surgeons are no different; they are technical virtuosos who must execute complex motor sequences under the gaze of a highly critical team. As the research suggests:
“Like musicians and athletes, surgeons must acquire vast technical knowledge and skills, and must utilise that expertise in front of an audience, namely the operating team members.”
The “Inverted U” and the Point of No Return
For decades, medical education has leaned on the Yerkes-Dodson law, the “Inverted U” theory which suggests that moderate stress optimizes performance. It is a comforting, gentle curve. However, for those in high-stakes environments, this model is dangerously simplistic. It fails to account for the cognitive toxin of worry.
A more frighteningly accurate representation is Hardy and Fazey’s Catastrophe Model. Here, the relationship between stress and skill is not a smooth arc but a cliff edge. If a surgeon’s “worry” remains low, they may follow the Inverted U. But when high cognitive worry meets high physiological arousal (the pounding heart, the sweating palms), the performer reaches a tipping point. Instead of a gradual decline, they experience hysteresis—a catastrophic, vertical drop in performance. Once the “catastrophe” occurs, a surgeon doesn’t just slow down; they can lose the ability to execute mastered motor tasks entirely, leading to iatrogenic risks like tissue damage or wound break-down.
Worry as a Cognitive Thief
The mechanism of this collapse is best explained by Attentional Control Theory. Anxiety does not just feel unpleasant; it is a “cognitive thief” that steals processing power. We must distinguish between processing efficiency—how hard the brain is working—and performance effectiveness—the actual outcome.
An anxious surgeon may still achieve a successful outcome (effectiveness), but they do so at a massive cognitive cost, forced to work twice as hard to inhibit internal distractors like negative thoughts or the perceived judgment of the room. This leads to the paradox of “self-focused attention.” When a veteran surgeon begins to consciously think about how they are tying a suture—a skill that should be as automatic as breathing—they disrupt the “automaticity” of the task. They begin to fumble like a novice precisely because they are trying too hard to be an expert.
“Worry acts as an internal distracter, attracting attention away from a current task and therefore reducing the capacity for attentional control.”
The Paradox of Perfectionism
The very trait that carries a student through the rigors of medical school—perfectionism—can become the catalyst for failure in the theater. Perfectionism acts as both fuel and poison. It is adaptive when it provides positive motivation and when the surgeon enjoys the pursuit of excellence. However, it becomes maladaptive when it shifts into excessive self-criticism and a fear of falling short of an impossible target.
The danger arises when a surgeon’s self-worth is fused entirely to the outcome of a procedure. In this state, perfectionism is no longer about maintaining standards; it is a “safety-seeking” behavior that maintains high levels of stress.
“Perfectionism may provide positive motivation and subsequently an increase in performance. On the other hand, if excessive, it may lead to performance-affecting levels of stress.”
Developing a “Surgical Shield”
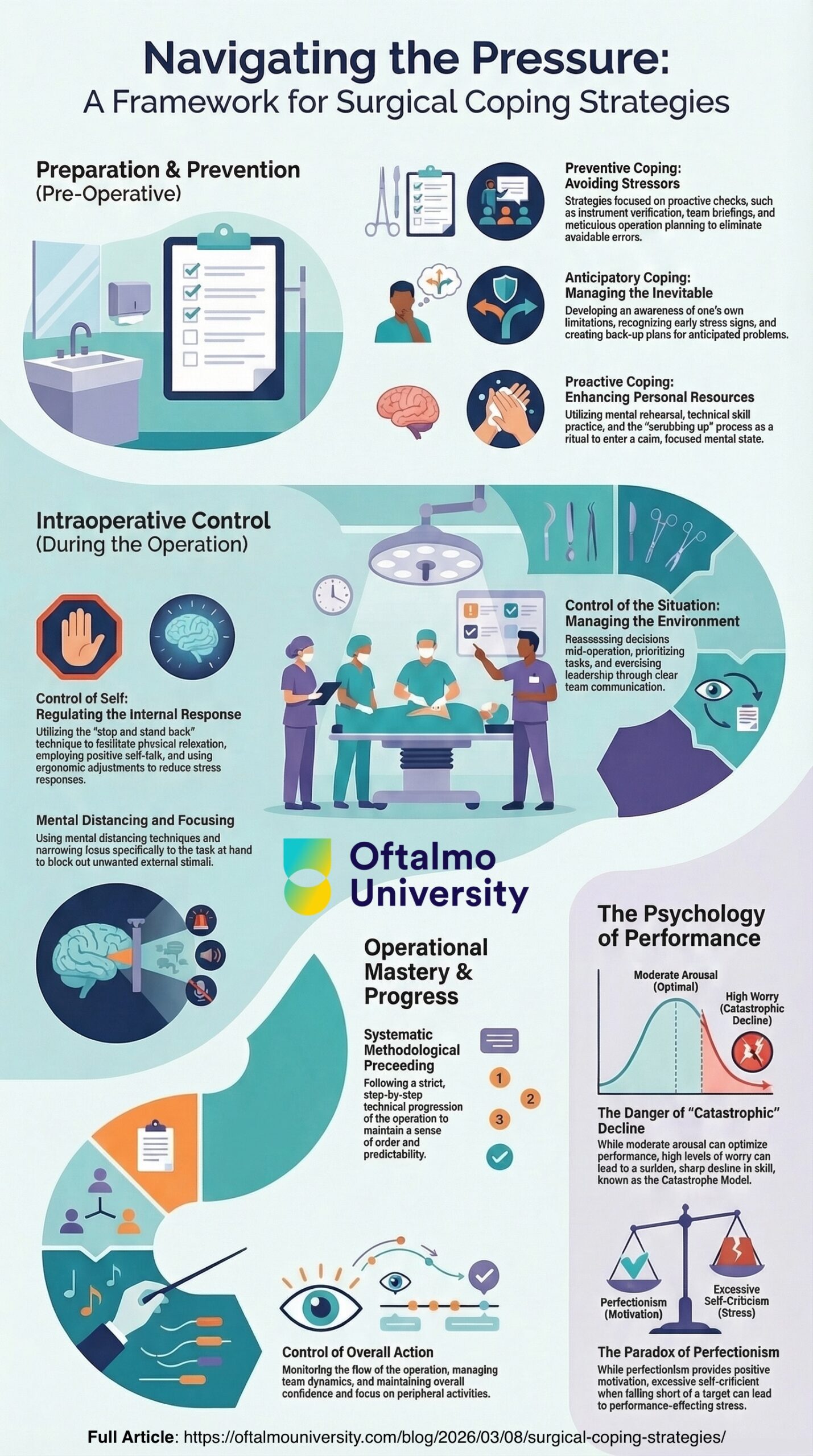
To survive the “catastrophe” cliff, elite surgeons develop a framework for resilience that spans their entire day. This is not a mere checklist but a “surgical shield” of coping strategies:
- The Prelude (Preventive & Anticipatory): Long before the first incision, the shield is forged through instrument checks, team briefings, and an honest acknowledgment of one’s own limitations. It is the “back-up planning” that prevents a minor equipment failure from triggering a cognitive spiral.
- The Airlock (Proactive): The “scrubbing up” process is utilized as a psychological reset, a ritual to enter a “different mode” of calm. It is a moment of mental rehearsal where the surgeon visualizes the systematic technical steps ahead.
- The Tactical Pause (Control of Self & Situation): Intraoperatively, the most effective tool is the “stop and stand back” technique. By physically stepping back, the surgeon facilitates physical relaxation and uses self-talk to reset the Catastrophe Model’s tipping point, regaining time to think before acting.
Crucially, we must distinguish these adaptive strategies—which increase focus—from maladaptive rituals. Maladaptive behaviors are driven by the superstitious belief that a disaster will occur if a specific ritual isn’t followed; these only serve to reinforce anxiety rather than manage it.
Beyond the Scalpel
Investigating performance anxiety is not a peripheral academic interest; it is a matter of professional survival and patient safety. In the UK, the rate of psychiatric morbidity among doctors is estimated to be between 17% and 52%. These numbers are not a reflection of personal weakness but a systemic failure to address the psychological toll of elite performance.
If we are to improve outcomes and stem the tide of burnout, we must move toward a medical culture where the mind is trained as rigorously as the hand. We must ask ourselves: How can we evolve our training to view performance anxiety not as a hidden shame, but as a manageable, predictable component of the surgical craft? Mastering the blade is only half the battle; the rest is mastering the mind that holds it.
INFOGRAPHY